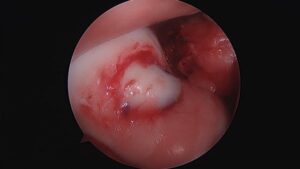
Mosaicplasty And Osteoarticular Allograft
Mosaicplasty is a one stage technique for treating small chondral or osteochondral defects where osteochondral plugs are transferred in to the defect from a relatively nonweightbearing area of the joint
Mosaicplasty
Autogenous osteochondral transfer for Osteochondritis dissecans was described initially by Yamashita (CORR 1985). Mosaicplasty or Osteochondral autograft transfer(OATS) involves transfer of small bone plugs covered with normal hyaline articular cartilage that are removed from a relatively nonweightbearing surface and transferred in a single stage to the chondral defect.
Advantages
- Defects can be filled immediately with mature, hyaline articular cartilage.
- The technique is also useful in osteochondral defects where there is bone loss.
- Good success rate in getting hyaline type cartilage.
Disadvantages
- Donor site morbidity is a concern and hence there is a limit to defect size treatable with this method. Hangody and Fuies recommend that the area to be treated is limited to between 1 and 4 cm 2
- The thickness of the donor cartilage may differ from that of the area to be treated and reconstitution of the important subchondral layer may not occur. In addition, lateral integration rarely occurs (Horas) raising the concern that synovial fluid may penetrate through the subchondral layer and cause cyst formation.
- Perpendicular access to the cartilage surface by cylinder cutters is required for this technique and this makes treatment of defects of the tibial plateau difficult.
- Mosaicplasty is not recommended on the patella (Bentley, Cole). Contact pressures of the patellofemoral joint make this a particularly challenging region with respect to osteochondral plug size, articular surface contour, and implantation technique (Garretson).
Biomechanics of Osteochondal plugs
Facts
- Larger plugs more stable
- Ideal length of plug=15mm
- Graft length and recipient hole should be equal length
- Multiple grafts less stable
- Chondrocytes die around the margins of plugs
Hangody showed that grafts of greater diameter are more stable in absolute values and there is no difference in primary stability between grafts implanted in a row or in circular fashion. Primary stability is better when grafts and drill holes are the same length, but if the recipient hole is shorter, excessive force must be exerted on the cartilage cup during insertion. Pull-out strength of press-fit plugs is directly related to the length and diameter of the plug; 15-mm-long plugs have a mean pull-out of 93 N, and, of those, 11-mm-wide grafts were significantly stronger (92 N) than were 8-mm-wide grafts (41 N). These pull-out strengths were reduced by half with graft reinsertion or levering at the time of harvest (Duchow). The plugs should be well seated and not proud as these lead to shear and micromotion. If the graft is sunk too much, then they would get covered by fibrous tissue. There is more forces and chondrocyte loss around the periphery of the plugs.
Multiple grafts may not be as stable as single grafts in the initial period after transplantation. There is substantial deterioration of short-term fixation strength of mosaicplasty grafts in the immediate postoperative period. Fixation strength of mosaic autografts decreased 44%, from 135.7 N to 75.5 N, over a 7-day period while soaked in a physiologic solution in vitro.
For cartilage defects within the weightbearing portions of the medial or lateral femoral condyles, grafts taken from sites from the most medial or lateral portions of the patellar groove provided a significantly better topographic match than did grafts taken from the central intercondylar notch.
Technique
The best donor sites for osteochondral plugs are medial or lateral edge of trochlea. An alternate site is edge of the notch. The whole procedure can be done through a small arthrotomy or arthroscopically, depending on the location of the lesion. Femoral condyle lesions are easier to deal with. Smith & Nephew and Arthrex have arthroscopic systems to perform this procedure. A sizer is used to determine the number and size of grafts that will be needed. The properly sized graft harvester with collared pin is introduced perpendicular to the donor site. It is lightly tapped into bone to a depth of approximately 12 to 15 mm . For removal, the harvester is twisted abruptly 90° clockwise and counterclockwise with a parallel pull to remove the donor plug. The harvester has a plunger that will push the donor plug into the recipient hole.
The recipient hole is created at a depth equal or 2 mm less than the donor graft just harvested and extracted in the same manner as the donor core. It is important to maintain a perpendicular relationship with the articular surface to create well-defined vertical walls in the recipient hole, which will facilitate congruent plug placement. This requires a constant knee flexion angle and often multiple accessory portals; implanting the graft plug immediately after harvesting will facilitate maintaining the proper insertion angle. The donor tube harvester is then placed over the recipient site, taking care to maintain perpendicular orientation, and the donor plug is gently advanced atraumatically into the defect, often leaving the plug slightly proud. Premature advancement of the plug before it is well seated in the recipient tunnel may result in loss of control of the plug and may require plug collection using loose body retrieval techniques. The final seating of the plug can be done with an oversized tap, taking care not to damage the articular cartilage on the surface of the plug graft. The final plug position should be flush with the surrounding articular cartilage. Graft congruence is key to minimizing shear.
Results
Results from Hangody
Hangody reported the results of operations on 597 femoral condyles, 76 tibial plateaux and 118 patellofemoral joints at up to ten years post-operatively. Good or excellent results were reported in 92%, 87% and 79% of patients who underwent mosaicplasty of the femoral condyle, tibial plateau and patellofemoral joint respectively. This paper does not give the mean time to follow-up and did not discuss the survival of osteochondral grafts in those patients with the longest follow-up
Longterm donor-site complaints measured by the Bandi score were minor and present only in 3% of patients. 81 out of the 98 control arthroscopies represented congruent and good gliding surfaces and histologically proven survival of the transplanted hyaline cartilage as well as fibrocartilage covering of the donor sites. Complications in the entire patient group were four deep infections and four deep venous thromboses. In nearly 8% of the cases excessive intraarticular bleeding was observed in the early postoperative period.
Multicentric, comparative, prospective evaluation of 413 arthroscopic resurfacing procedures (mosaicplasty, Pridie drilling, abrasion arthroplasty and microfracture cases in homogenised subgroups) demonstrated that mosaicplasty resulted in favourable clinical outcome in the long-term follow-up compared to other three techniques.
Results from other centres
Marcacci
Prospective evaluation of 30 patients (mean age, 29.3 years) with full-thickness knee chondral lesions (more than 2.5 cm (2)) treated with arthroscopic autologous osteochondral transplantation. 76.7% of patients had good or excellent results at 7-year follow-up, and International Knee Documentation Committee subjective score significantly improved from preoperative (34.8) to 7-year follow-up (71.8). The Tegner evaluation showed a significant improvement after the surgery at 2- and 7-year follow-up (from 2.9 to 6.2 and 5.6, respectively)
Bentley
100 patients with a mean age of 31.3 years and with a symptomatic lesion of the articular cartilage in the knee which was suitable for cartilage repair was randomised to undergo either ACI or mosaicplasty (58 ACI, 42 Mosaicplasty). Mean size 4.66cm2.and mean follow-up 19 months. 88% had excellent or good results after ACI compared with 69% after mosaicplasty. Arthroscopy at one year demonstrated excellent or good repairs in 82% after ACI and in 34% after mosaicplasty.
Horas
This is a prospective study with two-year outcomes in forty patients with an articular cartilage lesion of the femoral condyle who had been randomly treated with either transplantation of an autologous osteochondral cylinder or implantation of autologous chondrocytes. Improvement provided by the autologous chondrocyte implantation lagged behind that provided by the osteochondral cylinder transplantation. Histologically, the defects treated with autologous chondrocyte implantation were primarily filled with fibrocartilage, whereas the osteochondral cylinder transplants retained their hyaline character
Gudas
This prospective study looked at 57 athletes (28 OATS, 29 Microfracture). After 31 months 96% had excellent or good results after OAT compared with 52% for the MF procedure. Histology and MRI also showed better results with OATS.
References:
Yamashita F, Sakakida K, Suzu F. The transplantation of an autogeneic osteochondral fragment for osteochondritis dissecans of the knee. Clin Orthop. 1985;201:43-50
Zukor DJ, Oakeshott RD, Gross AE. Osteochondral allograft reconstruction of the knee, part 2: experience with successful and failed fresh osteochondral allografts. Am J Knee Surg. 1989;2:182-191.
Morelli M, Nagamori J, Miniaci A. Management of chondral injuries of the knee by osteochondral autogenous transfer (mosaicplasty). J Knee Surg 2002;15:185-90
Duchow J, Hess T, Kohn D. Primary stability of press-fit-implanted osteochondral grafts: influence of graft size, repeated insertion, and harvesting technique. Am J Sports Med. 2000;28:24-27
Whiteside RA, Bryant JT, Jakob RP, Mainil-Varlet P, Wyss UP. Short-term load bearing capacity of osteochondral autografts implanted by the mosaicplasty technique: an in vitro porcine model. J Biomech. 2003;36:1203-1208
Pearce SG, Hurtig MB, Clarnette R, Kalra M, Cowan B, Miniaci A. An investigation of 2 techniques for optimizing joint surface congruency using multiple cylindrical osteochondral autografts. Arthroscopy. 2001;17:50-55
Kordás G, Szabó JS, Hangody L. Primary stability of osteochondral grafts used in mosaicplasty. Arthroscopy. 2006 Apr;22(4):414-21
Hunziker EB, Quinn TM. Surgical removal of articular cartilage leads to loss of chondrocytes from cartilage bordering the wound edge. J Bone Joint Surg Am. 2003;85(suppl 2):85-92
Huntley JS, Bush PG, McBirnie JM, Simpson AH, Hall AC. Chondrocyte death associated with human femoral osteochondral harvest as performed for mosaicplasty. J Bone Joint Surg Am. 2005 Feb;87(2):351-60
Bartz RL, Kamaric E, Noble PC, Lintner D, Bocell J. Topographic matching of selected donor and recipient sites for osteochondral autografting of the articular surface of the femoral condyles. Am J Sports Med. 2001;29:207-212
Garretson RB III, Katolik LI, Verma N, Beck PR, Bach BR, Cole BJ. Contact pressure at osteochondral donor sites in the patellofemoral joint. Am J Sports Med. 2004;32:967-974
Hangody L, Kish G, Karpati Z, Udvarhelyi I, Szigeti I, Bely M. Mosaicplasty for the treatment of articular cartilage defects: application in clinical practice. Orthopedics. 1998;21:751-756
Hangody L, Fuies P. Autologous osteochondral mosaicplasty for the treatment of full-thickness defects of weight-bearing joints: ten years of experimental and clinical experience. J Bone Joint Surg [Am] 2003;85-A (Suppl 2):25-32
Hangody L, Feczko P, Bartha L, Bodo G, Kish G. Mosaicplasty for the treatment of articular defects of the knee and ankle [review]. Clin Orthop. 2001;391(suppl):S328-S336.
Alford JW, Cole BJ. Cartilage restoration, part 2: techniques, outcomes, and future directions. Am J Sports Med. 2005 Mar;33(3):443-60.
Results
Hangody L, Ráthonyi GK, Duska Z, Vásárhelyi G, Füles P, Módis L. Autologous osteochondral mosaicplasty. Surgical technique.J Bone Joint Surg Am. 2004 Mar;86-A Suppl 1:65-72
Bentley G, Biant LC et al. A prospective, randomised comparison of autologous chondrocyte implantation versus mosaicplasty for osteochondral defects in the knee. J Bone Joint Surg Br. 2003 Mar;85(2):223-30
Gudas R, Kalesinskas RJ et al. A prospective randomized clinical study of mosaic osteochondral autologous transplantation versus microfracture for the treatment of osteochondral defects in the knee joint in young athletes. Arthroscopy. 2005 Sep;21(9):1066-75.
Horas U, Pelinkovic D, Herr G, Aigner T, Schnettler R. Autologous chondrocyte implantation and osteochondral cylinder transplantation in cartilage repair of the knee joint: a prospective, comparative trial. J Bone Joint Surg [Am]2003:85-A:185-92.
OsteoArticular Allograft
Larger defects with previous failed treatment and those with significant subchondral bone defects are ideally treated with Osteoporosis-articular Allograft.
Trochlea Defect
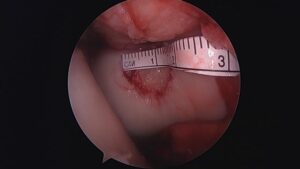
Prepared with Nanofracture
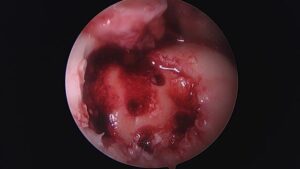
Allograft with Tissue Glue